Catching On To Keratoconus
- by Dr. Z Aleksic

- Apr 10, 2021
- 3 min read
The name ‘Keratoconus,’ probably because of its Greek derivatives, can be quite intimidating for patients, causing them to expect some rare and painful disease. The condition, however, is neither of these. Put simply, Keratoconus is an irregular shaped cornea, where ‘Kerato’ means cornea and ‘Conus’ means cone. If monitored and managed correctly, Keratoconus is a treatable condition.
The emphasis here is on monitoring. Because Keratoconus is a progressive disease of the cornea, it happens slowly, often from a young age and it therefore will have the best prognosis if the progression is monitored and stopped. It is also a hereditary disease, so it is crucial to take the whole family for a test if someone in it is diagnosed with Keratoconus, so that everyone’s progression can be dealt with immediately.
What happens to the eye with Keratoconus?
With Keratoconus, the cornea becomes thin and bulges outward, causing it to be irregular. This irregularity causes an inability to see clearly out of glasses and contact lenses. This mostly happens when you have a high amount of astigmatism (when the eyeball is not completely spherical) in the eye. The best analogy is to think of a normal eye as a half soccer ball, but an eye with Keratoconus will look more like half of an irregular rugby ball.
Diagnosing Keratoconus
There are some facts that may lead us to suspect that you may have keratoconus, which include family history, frequent need to rub the eye, allergies (hay fever, asthma or eczema) and astigmatism that constantly progresses, amongst others.
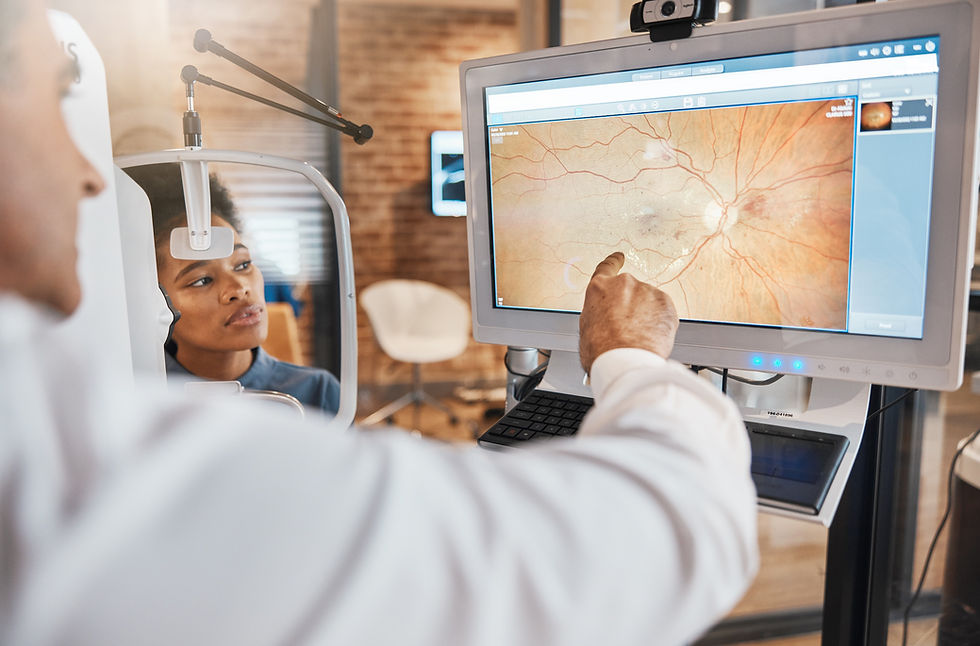
In order to confirm the diagnosis your eye doctor will look for signs in their slitlamp or microscope. The room in the image below is our Slitlamp examination room. This is where we use a high magnification microscope in order to view the anterior structures of the eye, in order to diagnose keratoconus, cataracts and various other pathologies. The same microscope will be used to evaluate the fit of a contact lens.

In the next step, your eye doctor will use a Pentacam to measure the topography of the eye. This is how we measure the thickness and regularity of the cornea. The Pentacam is a machine which is used to diagnose and monitor the progression of keratoconus. It can also give us information on whether or not you are a suitable candidate for laser refractive surgery.

Once Keratoconus is diagnosed, there are some necessary precautions which need to be made. Keratoconus is easier to be managed when found early. This is why it is essential to test the whole family if someone in the family is diagnosed with it. From diagnosis you will need an eye specialist to follow the progression, especially if diagnosed at a young age.
Corneal Cross linking
One of the treatments used to stop the progression of Keratoconus (in patients younger than age 40) is Corneal Cross Linking. When you are young your tissue is more pliable. This pliability is what allows Keratoconus to gradually gets worse, by letting the shape of the eye continue to progress into a cone. Thus, the goal of corneal-cross linking is to stop the progression. During Cross Linking your ophthalmologist will soak the eye in Vitamin B and tan the cornea by exposing it to UV light. This will stiffen the cornea and prevent progression of the disease. It is important to note that this treatment is not to make your Keratoconus better. It will not “cure” the condition or correct your vision, but instead the treatment is to stop the progression. The patient will then wear a bandage contact lens and can expect some scratching for a period of time.
Correcting your vision
The best way to correct your vision is by neutralising the shape of the eye using a hard or scleral contact lens. A hard lens moulds the cornea, whereas a scleral contact lens is a large lens which is used, and the gaps between the contact lens and the eye are filled with saline solution.
We have a series of explainer videos on our website for further queries:



Comments